Get Clients to “Yes” Faster With Instant Benefit Clarity
Here’s how verifying patient insurance eligibility with Reimbursify converts more consultations into committed clients:
Instant verification
Check out-of-network benefits in real time without logging into multiple portals or waiting on hold.
Clear financial picture
Show clients exactly what they’ll pay out-of-pocket and what their insurance will reimburse.
Reduced no-shows
When clients understand their financial responsibility up front, they are more likely to commit to treatment and show up for sessions.
Why Practitioners Choose Reimbursify
You became a therapist to help people, not to become an insurance billing expert. Understanding how to verify patient insurance eligibility shouldn’t require hours of training or complicated software. Reimbursify was built specifically to address the unique challenges out-of-network providers face.
Here’s what makes Reimbursify the right choice for your practice:


Reclaim Hours Every Week With Automated Verification
Manual benefits verification is a time sink. Between navigating payer portals and documenting everything, verifying patient insurance eligibility consumes hours each week — hours that should be spent seeing clients. Reimbursify’s OON benefits verification solution automates the entire process by connecting directly with insurance carriers to pull real-time eligibility data, deductible information and reimbursement rates into a centralized dashboard.
Experience faster intake, fewer errors, scalable growth and better work-life balance. Our insurance eligibility verification platforms free up time so you can focus on providing exceptional care to grow your practice.
Fast and Easy Reimbursement, Grateful Patients
(You’ll wish you had started using this sooner)

Never lose a prospective client again
Put the Reimbursify verification of benefits (VOB) calculator on your practice’s website and give clients peace of mind that they are covered for your services before they book an appointment.
Practitioners with our VOB calculator on their website see a 50% increase in first appointments booked.
Instantly provide clients accurate benefits insights
Not knowing who is eligible for reimbursement and who isn’t can result in less than expected paymentsleaving clients disgruntled and out of pocket.
It’s not your fault, but it’s reflecting badly on your practice.
Reimbursify’s real-time out-of-network benefits summary enables you to have educated conversations with your patients before treatment begins.

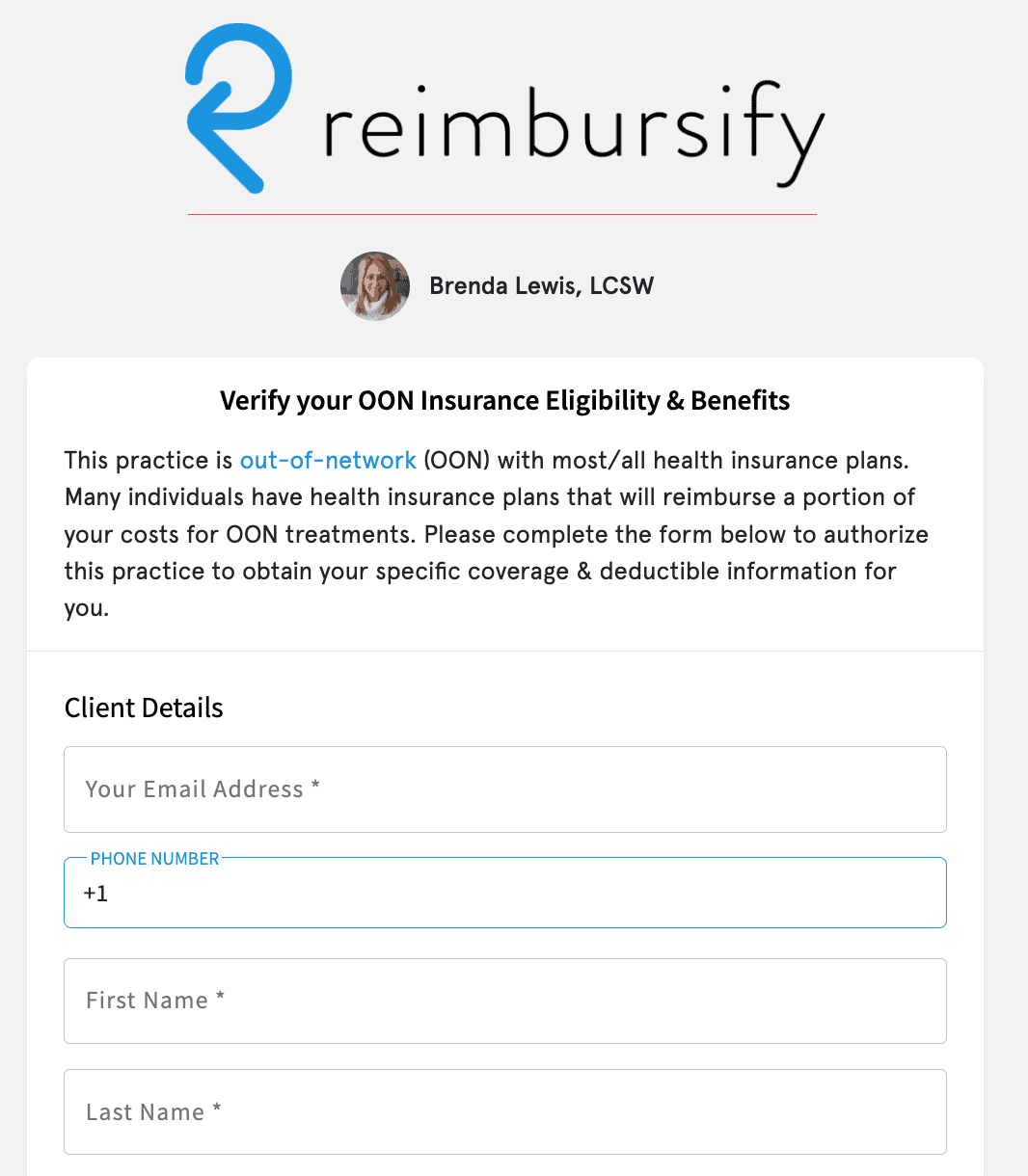

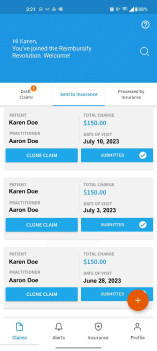
Effortlessly support your clients with reimbursement
Most clients find it difficult to navigate the out-of-network claim process. You want to help, but don’t have time to hand-hold. Reimbursify provides a courtesy claim filing feature via our Practitioner Portal, so that your practice gets all the benefits of patient insurance coverage with minimal extra work.
Waste less time dealing with insurers
Eliminate the hours you (or your admin staff) spend with insurers trying to determine your clients’ reimbursement amount or claim status. The Reimbursify client app puts all that information at your clients’ fingertips empowering them to manage the process themselves and freeing up your time.
Practitioners with Reimbursify save an average of 10hrs a month.

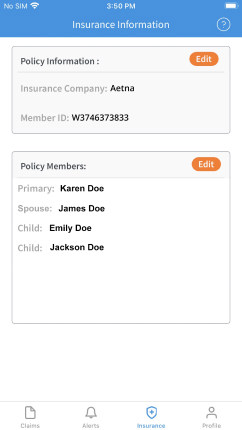

Don’t let rejected claims bog you down
A rejected claim usually ends up with a client reaching out to you to solve it. Reimbursify’s customer care team works directly with your patients to troubleshoot outstanding claims, so you can focus on delivering care.
Grow revenue and see your practice thrive.
Patients can drop out of treatment because they are not getting reimbursed. Reimbursify reduces claim rejections and gets clients reimbursed faster, which leads to fewer missed appointments and longer treatment relationships. Add our easy, low-cost billing solution, and you keep more of that revenue in your practice. Practitioners using Reimbursify often see their practice revenue grow by 15% or more.

Introducing the Reimbursify Practice Portal
Our cloud-based interface for managing your out-of-network patients and their insurance claims
Real-time verification of benefits (VOB)
Always know how much reimbursement a client can expect to receive for your services, including what their out-of-network deductible is and how much is remaining in their plan.
File claims on behalf of your clients.
No need to create superbills, you can file out-of-network reimbursement claims for a month of visits for a patient in as little as 10 seconds.
Verification of benefits (VOB) website calculator
Embed the power and simplicity of Reimbursify directly into your practice website, so that your clients can verify their benefits and file their own claims.
EHR and Practice Management Integration
Reimbursify integration can eliminate dual data entry and speed up the process for everyone.
Easy claim filing for clients.
Claims can be self-filed by your patients with either the Reimbursify mobile app or right from your practice website with our FileFAST button.
Manage reimbursements all in one-place
See who is filing for your services and how much reimbursement they are receiving. Manage your solo or group practice profile, including locations, practice information, NPIs and practitioners to optimize reimbursements for your caseload.
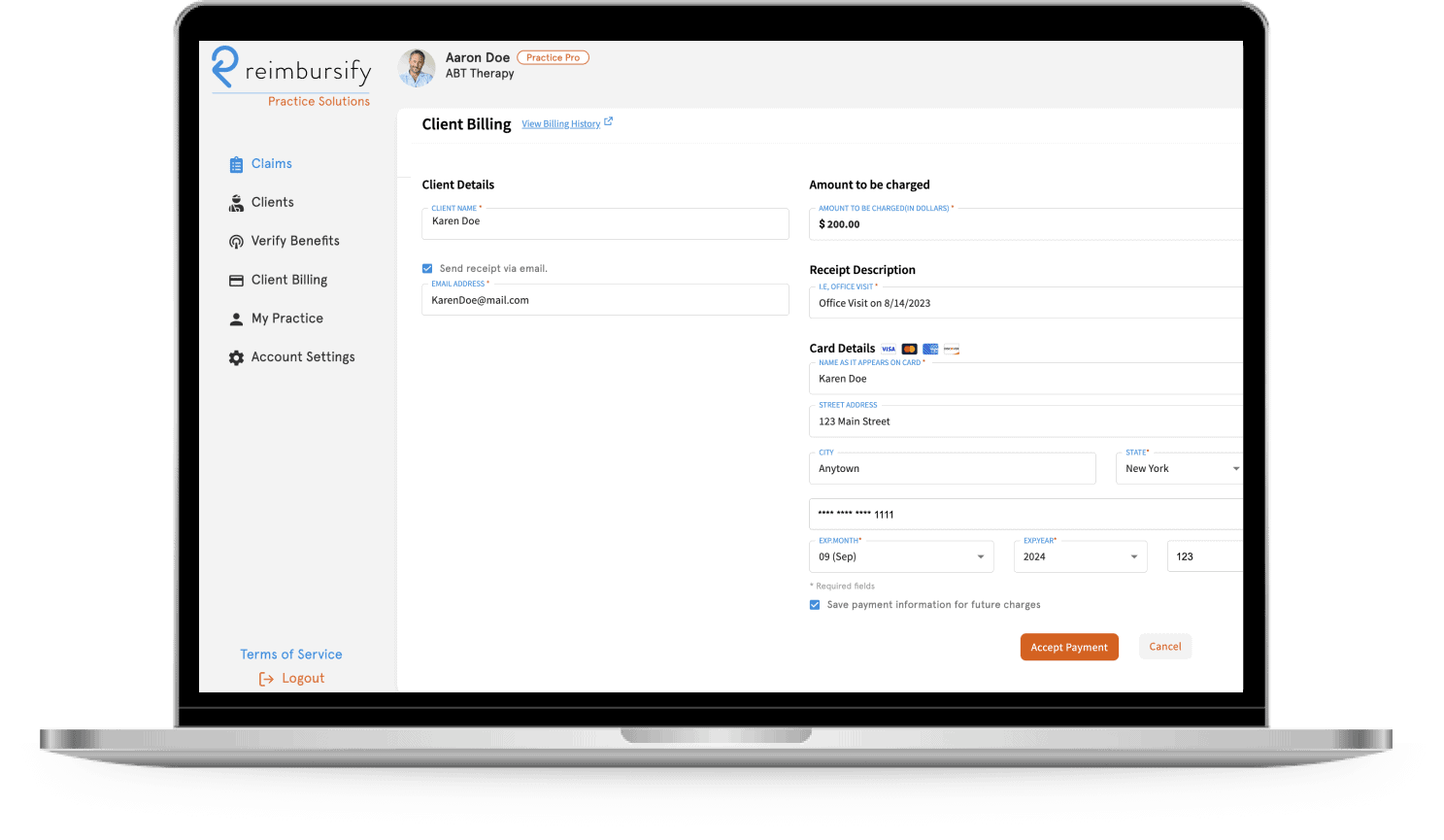
Secure, low-cost credit card payment processing
Store clients’ credit card information so payment takes only a couple clicks. Receipts are sent automatically and reimbursement claims are filed immediately after you are paid. You can charge clients after each visit or monthly and funds are deposited into your bank account within 2 business days.
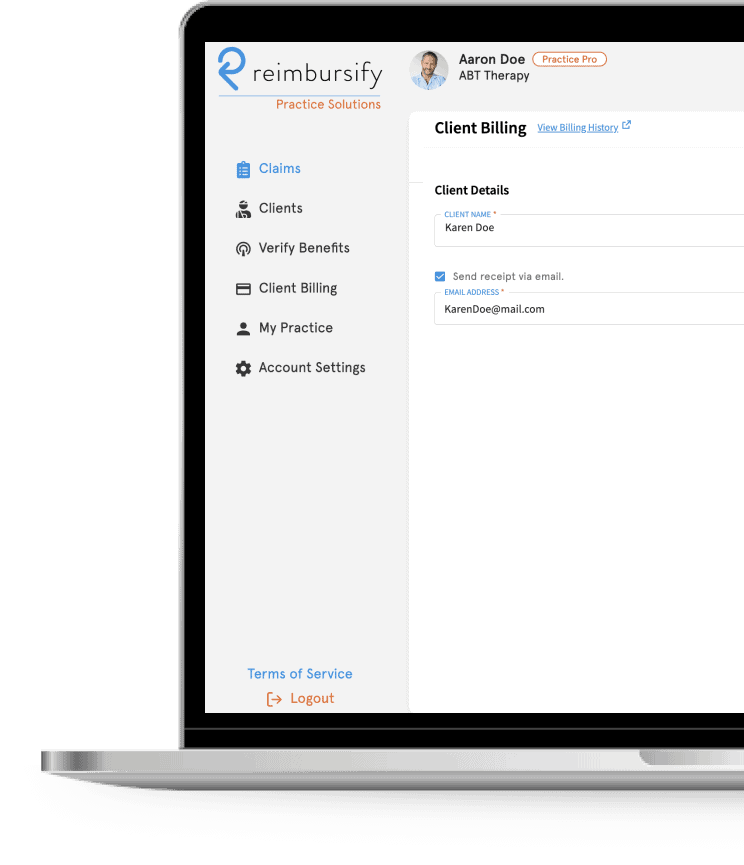
Build Trust That Keeps Clients Engaged
Out-of-network reimbursement feels like a black box to clients. When you can’t provide clear answers about their benefits, their uncertainty grows. Reimbursify’s verification of benefits software empowers you to have transparent, confident conversations about costs from day one. You’ll show clients their deductible status, explain their reimbursement percentage and help them understand what to expect at every stage.
This transparency builds trust and increases retention. Clear financial expectations eliminate stress, satisfied clients refer friends and family, and you create a seamless experience that sets your practice apart from in-network alternatives.
Start Verifying Benefits in Minutes
Stop spending your time on the phone with insurance companies. Reimbursify gives you the freedom to provide exceptional care on your terms. Our verification of benefits platform works the way you do — quickly, accurately and without unnecessary complexity.
Ready to simplify your practice and attract more private-pay clients? Explore our pricing plans or speak to an expert to learn how Reimbursify transforms your verification process.
Take complete control of your out-of-network reimbursement claims
Get out-of-network reimbursement running like clockwork with Reimbursify