File a Month of Claims With a Single Click
With Reimbursify’s courtesy filing feature, you can submit claims for multiple sessions simultaneously through your Practice Portal. Select the sessions you want to bill, review the pre-populated information, and submit everything in one go. Automated formatting, built-in validation and direct transmission to insurance carriers happen instantly.
Know Exactly Where Every Dollar Stands
The worst part of claim filing isn’t the submission — it’s the waiting. Clients ask when they’ll get reimbursed, and you have no answer because you’re stuck waiting for insurance companies to process paperwork.
Our insurance claims management system provides complete transparency throughout the entire process:


Protect Clients From Surprise Denials
Nothing damages client trust faster than an unexpected claim denial weeks after treatment. Out-of-network claim patient protection is built into every step of Reimbursify’s process. Our insurance claims platform validates all claim data before submission, catching errors that would cause automatic denials. We verify that diagnosis codes match treatment codes, confirm that patient information aligns with insurance records, and ensure all required fields are complete. Reimbursify’s comprehensive approach safeguards your practice’s reputation and your clients’ financial expectations.
Add Clients Without Adding Chaos
More clients mean more revenue — but only if your administrative systems can handle the growth. The insurance claims management system you implement now will determine whether expansion feels sustainable or suffocating.
Our solution covers essential capabilities for growing practices:
Batch processing: Submit dozens of claims simultaneously without multiplying your workload.
Automated record-keeping: Every claim submission includes timestamps, confirmation numbers and status history stored permanently.
EHR compatibility: Pull session data directly from your existing systems to eliminate redundant data entry.

Fast and Easy Reimbursement, Grateful Patients
(You’ll wish you had started using this sooner)

Never lose a prospective client again
Put the Reimbursify verification of benefits (VOB) calculator on your practice’s website and give clients peace of mind that they are covered for your services before they book an appointment.
Practitioners with our VOB calculator on their website see a 50% increase in first appointments booked.
Instantly provide clients accurate benefits insights
Not knowing who is eligible for reimbursement and who isn’t can result in less than expected paymentsleaving clients disgruntled and out of pocket.
It’s not your fault, but it’s reflecting badly on your practice.
Reimbursify’s real-time out-of-network benefits summary enables you to have educated conversations with your patients before treatment begins.


Effortlessly support your clients with reimbursement
Most clients find it difficult to navigate the out-of-network claim process. You want to help, but don’t have time to hand-hold. Reimbursify provides a courtesy claim filing feature via our Practitioner Portal, so that your practice gets all the benefits of patient insurance coverage with minimal extra work.
Waste less time dealing with insurers
Eliminate the hours you (or your admin staff) spend with insurers trying to determine your clients’ reimbursement amount or claim status. The Reimbursify client app puts all that information at your clients’ fingertips empowering them to manage the process themselves and freeing up your time.
Practitioners with Reimbursify save an average of 10hrs a month.


Don’t let rejected claims bog you down
A rejected claim usually ends up with a client reaching out to you to solve it. Reimbursify’s customer care team works directly with your patients to troubleshoot outstanding claims, so you can focus on delivering care.
Grow revenue and see your practice thrive.
Patients can drop out of treatment because they are not getting reimbursed. Reimbursify reduces claim rejections and gets clients reimbursed faster, which leads to fewer missed appointments and longer treatment relationships. Add our easy, low-cost billing solution, and you keep more of that revenue in your practice. Practitioners using Reimbursify often see their practice revenue grow by 15% or more.

Introducing the Reimbursify Practice Portal
Our cloud-based interface for managing your out-of-network patients and their insurance claims
Real-time verification of benefits (VOB)
Always know how much reimbursement a client can expect to receive for your services, including what their out-of-network deductible is and how much is remaining in their plan.
File claims on behalf of your clients.
No need to create superbills, you can file out-of-network reimbursement claims for a month of visits for a patient in as little as 10 seconds.
Verification of benefits (VOB) website calculator
Embed the power and simplicity of Reimbursify directly into your practice website, so that your clients can verify their benefits and file their own claims.
EHR and Practice Management Integration
Reimbursify integration can eliminate dual data entry and speed up the process for everyone.
Easy claim filing for clients.
Claims can be self-filed by your patients with either the Reimbursify mobile app or right from your practice website with our FileFAST button.
Manage reimbursements all in one-place
See who is filing for your services and how much reimbursement they are receiving. Manage your solo or group practice profile, including locations, practice information, NPIs and practitioners to optimize reimbursements for your caseload.
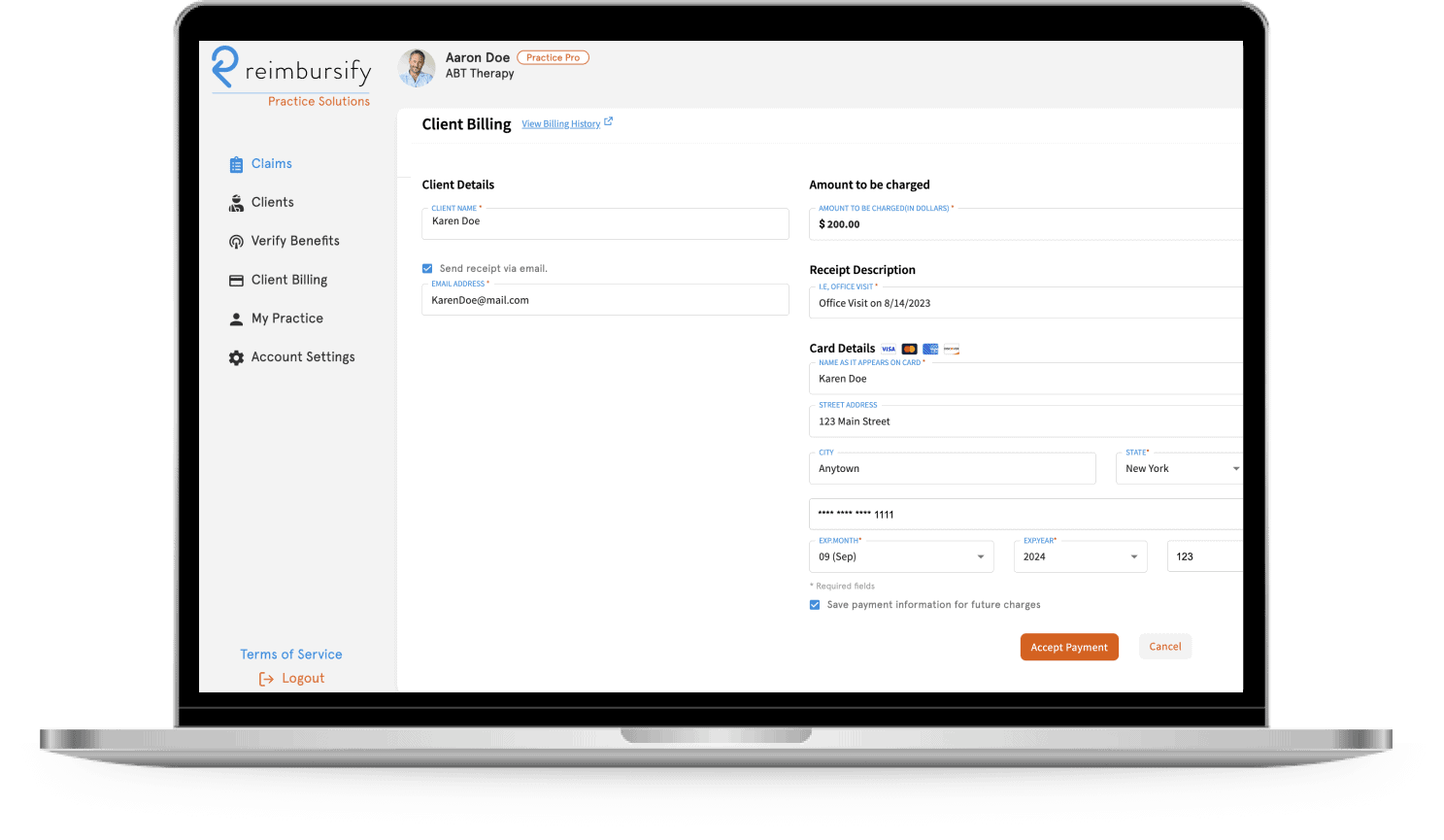
Secure, low-cost credit card payment processing
Store clients’ credit card information so payment takes only a couple clicks. Receipts are sent automatically and reimbursement claims are filed immediately after you are paid. You can charge clients after each visit or monthly and funds are deposited into your bank account within 2 business days.
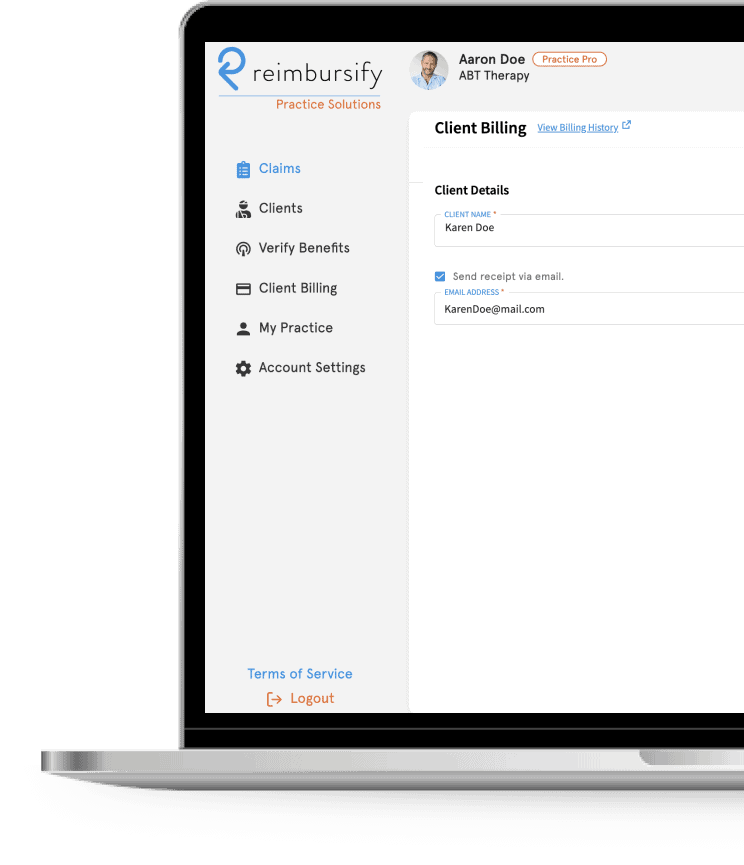
Stop Being Your Clients’ Insurance Navigator
When clients file their own claims manually, they inevitably run into problems. They’ll call asking which codes to use, how to fill out forms, or what to do when a claim gets denied. These interruptions pull you away from clinical work.
Automatic claim filing and tracking removes you from that equation entirely. Whether you file courtesy claims on behalf of clients or empower them to file through the Reimbursify app, built-in guidance walks them through every step. Reimbursify’s dedicated support team handles troubleshooting, not yours.
Start Filing Claims the Modern Way
Reimbursify’s insurance claims software handles the administrative complexity, so you can focus on providing transformative care. View our plans and see how automatic claim filing and tracking can transform your practice workflow.
Take complete control of your out-of-network reimbursement claims
Get out-of-network reimbursement running like clockwork with Reimbursify